Healing at Home
I was discharged from the hospital exactly a week ago today.
The way time has been showing up like an elusive guest with too much news and very little of itself to give, this week has sped by. I’m surprised because I’ve primarily been on my sofa trying to stave off the intense pain and deep discomfort that comes with not being active. I sleep when I can, which isn’t restorative or even restful. Lying on my back (which is the only way I’m supposed to lie, to the dismay of the sidesleeper I’ve been my whole life) just brings more phlegm that my lungs try to violently push out. I’ve awakened too many times to count, hanking uncontrollably and nearly choking; too afraid to go back to sleep. My breasts feel heavier than ever before and it feels like someone is stepping on my chest.
In the hospital, they taught me about splint coughing, which just means gripping a pillow or rolled-up towel to my chest as tightly as possible to offset the pressure of the coughing on my chest and incision. When I was transferred out of ICU into my room on the step-down cardiac floor, a sweet volunteer for the cardiac surgical program named Diane was one of the first people to visit me. She’s 82, and she shared that she had 2 open heart surgeries over the years. Diane told me to remember that I will not always feel as awful as I did then/do now - that soon my healing will be apparent and my mind will start to convince me that I get back to business as usual, and ignore my restrictions. I can’t say I didn’t have this fear going into this; it’s just how I am: always pushing to do exactly what I want when I want. But she told me to exercise patience and take time to heal as to not make things worse. Diane gave me a purple heart pillow to grip when I cough, and it is my reminder to not rush any of this post-surgical restoration. The way the hours speed by, each day my incision is visibly healing, it is demonstrating the fleeting nature of time. Soon I’ll be 6 months out, well back at work, getting around on my own, socializing, and taking care of my home again. Soon.
But for now, despite my discomfort, I’m just so relieved and happy to be at home. Especially when I think about how afraid I was of not making it through the procedures. Everything was as I’d left it, the smell and the feel still comforting. I’m surrounded by flowers from my dear family and friends, some of which I brought with me from the hospital. I have to recognize how much I am loved and cared for; I’ll remember this time as the most poignant example.
My days at home so far are defined by my discharge instructions. I’m to shower and walk every day, which seems simple enough, but it can be a struggle; it certainly spends my energy quicker than I realize I have it. When I shower (which I’m able to do without supervision now), I have to face away from the stream, and I’m supposed to keep the water temperature cool and the shower itself short, but my delight in a hot, long shower has lately been winning in that way. I’m monitoring my incision, and it seems to be healing just fine. I’m to gently wash my incision last with the cleanest cloths and mildest soap. Then, after, I pat it dry very gently. The Physician Assistant on my case told me that it was imperative to get my incision as dry as possible, so he suggested using a hair dryer on cool, and this has been working brilliantly. I’m still wearing surgical bras; not the most comfortable, but they hold everything in place as they should. In addition to an almost 7-inch incision, I have scars from drain tubes on my chest, right above my stomach. I had my drain in for the full time I was in the hospital, and I cannot express how happy I was for them to remove it right before discharge. In another post, I’ll go in-depth about my incision and share photos so you can get an idea of what I’m dealing with. It’s odd (maybe not) that there’s not a minute that goes by that I’m not thinking about my incision. I suppose I’m obsessed.
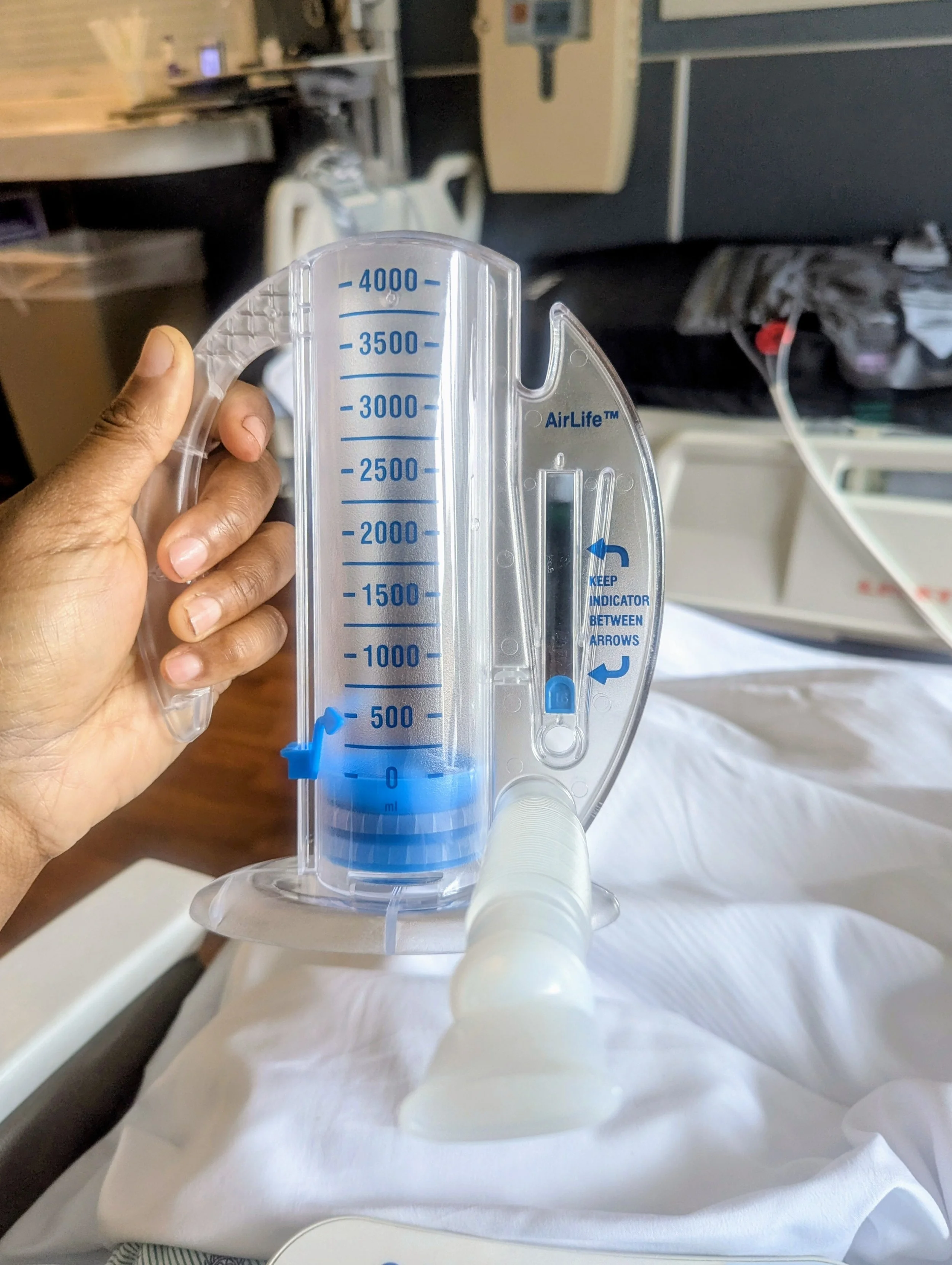
They sent me home with a spirometer to work out my lungs. The type of surgery I had can leave the lungs weakened and full of phlegm (hence the coughing), so I’m to use my spirometer 10x an hour. Now, am I managing to do that? Not at all. I keep it out on the table next to me as a reminder, but I’m probably using it every other hour. I’m to suck into this plastic thing, and a piece moves up a gauge to tell me how much I’m aspirating. So far, I haven’t been able to get past 1000ml….hold on, I’ll be back, I’m going to use it now.
Now, I’m only getting up to 500ml. I do realize how much breathing has suffered post-surgery, and I can only hope it starts getting better very soon. When I take my walks, I get winded immediately. Mind you, I’m walking as slowly as possible, leaning on my boyfriend. Sometimes I even have to stop completely to catch my breath. This is super frustrating for me; more than I thought it would be. Again, I’m hell-bent on getting back to normal, and not being able to walk more than a block without wheezing is the harshest evidence that this will take time. I fear for the day I’m out alone and I get winded and there’s nowhere to sit. People can’t see my damage unless I show them, and I fear the general public won’t be understanding because I appear able-bodied.
Here’s a general list of my restrictions for the next few weeks:
Don’t lift more than 10 lbs
Don’t push or pull with my arms (this includes getting up from sitting, opening doors, etc)
Don’t raise both arms over head at the same time (this makes doing my hair and getting dressed a challenge)
Don’t put both arms behind back at the same time
Don’t sleep on sides or stomach
I admit, I have violated these restrictions a few times, but it shouldn’t do any long-term damage. I mean, I feel in my chest and incision when I’m lifting my water bottle when it’s full, and it’s not even 10 lbs. I think the lifting restriction will be the easiest to follow. But I have supported my own weight with my arms getting up, and that hurts like hell. They told me to cross my arms over my chest and use my core and legs to get up, which I’m getting better at. I have been sleeping on my side because I don’t know how else to get comfortable enough to fall asleep. Ultimately, I have been sleeping on my back more if I don’t cough too much. A few times during the night, I have to sit up and try to sleep because it’s the only thing that relieves the coughing. This puts a lot of strain on my neck, but it’s a price I’m willing to pay for good sleep.
Medication
Oh, all the pills! I’m definitely on less than I was in the hospital. They had me on 3 painkillers and a muscle relaxer right after surgery. There was a button I could press to get one of the strongest ones. There were certainly restrictions with that, but if I looked down at it and it was green, hey, now! The nurses took me off that when I left ICU because they said I was pressing it often, so that was a good sign. Honestly, I think I was just weak and overwhelmed by all the medical personnel coming in and out of my room that I just forgot to press it. The muscle relaxer helped me get comfortable enough to sleep, and then I was on Oxycodone and Tylenol. I have to take diuretics because of the Oxy (it can cause constipation with repeated use). They also put me on a new blood pressure medication, Aspirin to prevent clotting, and big ass potassium pills because the diuretics can lower potassium levels, which can wreak havoc on your blood pressure.
At home, I’m still on the Oxy and Tylenol for pain, the diuretics, Aspirin, blood pressure pill, potassium, and a multi-vitamin. Pain management has been tricky: I have really good moments, then really horrible ones. I’m to wean off the Oxy soon, as my prescription was only for 8 days (which my janky insurance refused to cover because they only cover 7 days). I have decreased the amount I take during the day, replacing it with doses of Tylentol so that I can take 2 Oxys at night with the hopes of getting knocked tf out. It puts me out for a couple of hours before I’m up again, coughing. The pain isn’t as intense closer to the time I take it, but as the night goes on, I notice it hurts more. I have 2 more nights of Oxy, and then it’s Tylenol only. Then I don’t have to take the diuretics! Fewer pills = happier me.
I have to monitor my blood pressure and weight twice daily. Because of my history of disordered eating, I stopped monitoring my weight years ago, and only knew how much I weighed if I went to a doctor’s appointment. I was initially hesitant to bring a scale into my home, but after going through all this, I ordered one with no issue. I have to track my weight because significant weight gain after invasive surgery can indicate fluid building and retention, which is not good. In the ICU, my bed would take my weight, then once I was in step-down, they’d wheel a big ol’ scale in that I’d stand on. It does feel satisfying to have control over more of my care at home. I write down my blood pressure readings and weights so that I can share them with my doctor when I have my appointments. Or they call and ask me. This method allowed me to decline home nurse care, which I didn’t want to pay for. I have to get weekly blood draws, but there’s a facility close to me that I can go to for that. So far, everything looks good.
Taste
The last thing I’d like to discuss is my sense of taste post-surgery. This has perhaps been the most understated surprise that’s proving to be a huge challenge. I was complaining about the hospital food tasting acrid and bitter, but that was actually my tongue. My boyfriend researched and found that people can lose or experience changes in their sense of taste after invasive surgery. I feel I owe the Northwestern Hospital chefs a huge apology because I clowned their food until my final meal there which actually didn’t taste too bad. Maybe it’s mental, I don’t really know. But at home, my food initially tastes ok but then that bitterness sets in. It’s really affecting my desire to eat or finish a meal. I wasn’t eating much in the hospital, yet I was so bloated and gassy from the surgery; I’d put on 8 lbs from the last weight they took before my procedure. Now at home, I’m 10 lbs down from that initial weight. This isn’t something I could’ve ever expected, but invasive surgery really does screw with your whole body. Hopefully, my taste comes back soon because I am hugely food-motivated, and I want to start cooking again as soon as I can. But for now, I’ll be here on the couch, except when my boyfriend takes me out for walks or when I’m in the shower.
I’m Having Surgery
A week from today.
No one has asked me if I’m ready because I’ll never be, and they already know that. I mean, I’ve had several pre-op appointments and tests over the past few months. My attendance to those was stellar. I asked questions, and I think I remember hearing answers. I got bloodwork; 7 vials taken leaving me confused and dizzy in the hospital concourse. I had to fast before the labs which were in the middle of the afternoon. This left me so disoriented that I purchased an $18 salad at the salad bar. I’d never do that in my right state of blood. I should be able to write that salad off. And my transportation to and from downtown over the past 10 years, while they figured out what to do with my conditions.
In times like these, I become effective. I manage. I schedule and order things. I check in with my close ones and communicate my needs. I do everything to stave off anxiety, but eventually end up succumbing. It always catches up to me. Whether it’s at work and I’m at my desk having an unremarkable day, or at 4am when I’m shocked awake by the thought of dying on the table with my heart and innards exposed to a blank ceiling.
In times like these. Well, I’ve never had times like these. I’ve never had invasive surgery. My doctors have been doing everything to manage it all from the outside. Foreign climbs that many have traversed; just not me. And not like this. During my preparation, I did what any self-respecting American who pays into this scam ass insurance system would do: I googled my conditions + treatment and then eventually +surgery. Reddit threads, cardiac forums, and youtube opened up an aggregate of stories from previously cut-open patients detailing their experiences, ranging from regret to relief. One person said they suffered permanent nerve damage from one of the procedures I’m having. I immediately turned off my phone, rolled over, and shut my eyes tight, trying to squeeze out that person’s story cemented behind my lids in text. I can still see the shape of the paragraph.
What am I having? Excellent question. The answer to it I’ve repeated so many times and in different ways to anyone inquiring. Each time, you’d think I’d understand more about it, but it just gets heavier with each sympathetic look I get in response. It’s hard to tell people that something’s wrong with you. You’ll get those sympathetic looks coupled with “it’ll be okay.” Or, most aggravatingly, they’ll change the subject out of discomfort. I can’t say I don’t understand, though. Something’s wrong now, but they’ll fix it, right? I mean, is that the point of all of this? That’s how I choose to see it, like a little wrench icon that pops up for me to click. Even though one of my doctors told me they can’t guarantee optimal results.
In a week, I’m having primary Tricuspid Valve (TV) repair and chest wall reconstruction to correct Pectus Excavatum. My doctors believe both of these procedures will increase the quality and length of my life. I suppose I believe it too, even though my conditions aren’t necessarily interrupting my life. They are responsible for the decrease in the tolerance I have for physical activity. I had quit dancing and eventually biking because I just couldn’t keep up. Low-impact activity isn’t an issue as long as I’m not in AFib (which I also deal with.) Basically, my heart works much harder than average to do what everyone else can do easily.